4 innovations for an antibiotic-free future
With antimicrobial resistance (AMR) increasingly preventing effective treatment of bone infections with antibiotics, innovative non-antibiotic therapies such as bioactive glass-based solutions are ever more in demand. Osteomyelitis remains a serious condition with cases globally increasing, and antibiotic-free treatments may offer a future with sustainable solutions widely available.

Bone infection cases on the rise
Bone infection, also called osteomyelitis, is an inflammatory disease of the bone marrow caused by infectious pathogens.1 Bone infections are microbial infections that can be either acute complications following trauma or surgery, or chronic conditions developing slowly over time.2, 3 Recurrent and persistent infections occur in approximately 40% of patients.4 In children, the infection usually concerns the long bones of arms and legs, while in adults the spinal vertebrae, hips, and feet are most commonly affected.1
Osteomyelitis remains a serious, potentially destructive infection
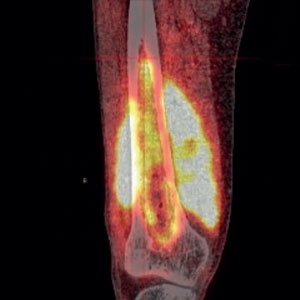 Bone infection is a prevalent disease affecting males more often than females, especially after 60 years of age.1, 2, 5 It was common before the invention of antibiotics and even though morbidity has dropped to 3%, it is still globally significant and the disease remains a challenge to treat.6 In addition, in a study conducted in the United States, osteomyelitis cases were increasing and had doubled from the 1970’s until the early 2000’s due to factors including changes in diagnostics and a significant increase in diabetes-related and vertebral bone infections.5
Bone infection is a prevalent disease affecting males more often than females, especially after 60 years of age.1, 2, 5 It was common before the invention of antibiotics and even though morbidity has dropped to 3%, it is still globally significant and the disease remains a challenge to treat.6 In addition, in a study conducted in the United States, osteomyelitis cases were increasing and had doubled from the 1970’s until the early 2000’s due to factors including changes in diagnostics and a significant increase in diabetes-related and vertebral bone infections.5
Picture: PET-CT of chronic osteomyelitis in the distal femur. Courtesy of Infection Unit, Maastricht UMC+, the Netherlands.
Infection sources include more resistant bacteria
The major sources of bone infection are hematogenous spread, resulting from an infection that is transported through the bloodstream to a bone in a distant location, and direct pathogenic inoculation from trauma or surgery.1, 2 If left untreated, the infection leads to progressive bone destruction and loss.5
Osteomyelitis is most commonly caused by the bacterium Staphylococcus aureus, but also Staphylococcus epidermidis, Streptococcus pneumonia, and Streptococcus pyogenes are common pathogens.1, 2, 4, 5 More resistant strains have emerged due to growing antimicrobial resistance (AMR), and the main pathogens are slowly changing from gram-positive to gram-negative bacteria.1
Innovative non-antibiotic antimicrobial approaches are vital
Risk populations include people with diabetes, hemodialysis patients, and intravenous drug addicts.2 Bone infections of the foot are common in people with diabetes. The lifetime risk of people with diabetes to develop a foot ulcer is 34%, and more than half of these ulcers become infected7. A further 20% of diabetic foot infections result in amputation8. Specialists state that these amputations are largely preventable, yet 50% of these patients die within 5 years of the procedure.9, 10, 11, 12
Innovations for the treatment of bone infections
Bone infections have traditionally been treated with large doses of pathogen-appropriate antibiotics, both intravenously and locally, and depending on the extent of the infection, with surgical cleaning of the affected area. Bone grafts are sometimes necessary as well.2 The diagnosis and treatment of osteomyelitis have improved over the previous decades with advances in bone regeneration, the development of new antibiotics, and improvements in vascular surgery and trauma care.5
Nevertheless, osteomyelitis remains a serious, potentially destructive infection, especially in diabetes-related diabetic foot infection cases. Antimicrobial resistance (AMR) is increasingly having a negative effect on the response to treatment of bone infections, which is why innovative non-antibiotic antimicrobial approaches are vital in developing future treatment solutions.
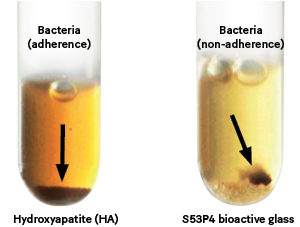
Picture: Bacteria test with pigmented Porphyromonas gingivalis shows that bacteria cannot adhere or grow on S53P4 bioactive glass. 13
Potential future therapy solutions could be based on the following technologies:
- Bioactive glass
Bioactive glass acts as a bone graft substitute for filling, replacement, or reconstruction of bone defects. The bioactive glass composition S53P4 naturally inhibits bacterial growth, even MRSA and MRSE, making it a smart and sustainable solution for infection treatment and bone regeneration. 14, 15, 16, 17 The Bonalive® S53P4 bioactive glass granules are already used in infection treatment and bone regeneration applications in septic bone surgery with proven good long-term results. 18
- Metals
Many metals possess antimicrobial properties, including silver, iron, tellurium, copper, and zinc. While their microbe-targeting mechanisms are only partially known, metals have proven to be potential antimicrobial agents against drug-resistant bacteria.4
- Polymers (chitosan)
Chitosan is a linear, natural polysaccharide that is most commonly derived from the shells of crustaceans. It is biodegradable, biocompatible, and nontoxic and displays antimicrobial activity. Chitosan is often combined with metal ions.4
- Peptides
Antimicrobial peptides (AMPs) are short proteins that form part of the human immune system. Some antimicrobial peptides, for example LL-37, demonstrate vast antimicrobial activity and promote bone regeneration.4 Synthetic peptides called Synthetic Antimicrobial and Antibiofilm Peptides (SAAPs) kill antibiotic resistant strains within hours and are not associated with resistance development. They can also prevent and eradicate biofilms and persister cells.19
Prerequisites for a successful treatment
Successful treatment of bone infections always depends on proper debridement of infected tissue and surgical resection of any necrotic bone and/or removal of prosthetic implant. While some of the aforementioned technologies will reach the market as clinically available solutions, some may not. Bonalive® granules is a bacterial growth inhibiting material available for bone cavity filling in the treatment of chronic osteomyelitis.
➡ Sign up to our quarterly newsletter.
➡ Read about cost-effective bone infection surgery using Bonalive® granules.